- Blog
- Icloud Generator V3.2.1
- Chupulu Kalasina Subhavela Serial All Episodes
- Doraemon Episodes In Hindi 2012 Free Download
- Bacaan Doa Sholat Tahajud Pdf
- Medison Sa 600 Manual
- Intel Q35 Chipset Host Embedded Controller Interface Driver
- Animezeria One Piece Season 17
- Descargar Libro Cloud Atlas Espanol Pdf
- Vag-Com Release 409.1 For Modern Serial Interfaces
- Dell Sigmatel Audio Driver Windows 7
- Download Download Tunerpro Definition Files Free
- Baixar Driver De Rede Realtek Nicdrv_8169 Win7
- Install Solaris On Kvm Qemu
- Boldbeast Call Recorder Cracked Version Of Snapchat
- American Pie Hindi Dubbed Movie Download
- How To Pass Japanese Drivers Test
- 24 Mani Neram Tamil Movie Mp3 Songs Free Download
- Remove Xml Version= 1.0 Encoding= Utf-8 From Xml C#
- Windows 98 Nes Rom Download
- Castlevania Rondo Of Blood Snes Rom
- Venkatachalapathy Mp3 Songs In Tamil
- Hayley Westenra Paradiso Rar File
- Vamsam Serial Roja Facebook
- Mailbox Has Been Temporarily Moved On Microsoft Exchange Server
- Body By Science Mcguff Pdf Creator
- Rgh xbox one 2016
- Epson wf 3640 driver
- Wansview app on multi pcs
- Arkaos grand vj 1-2
- Xiaopan os
- Thought field therapy migraine algorithm
- Dr cleaner pro cracked
- Uberstrike shotgun
- Refurbished flip video camera
- Voicemod pro free 2021
- Mario kart 8 best kart
- Jinke marina song
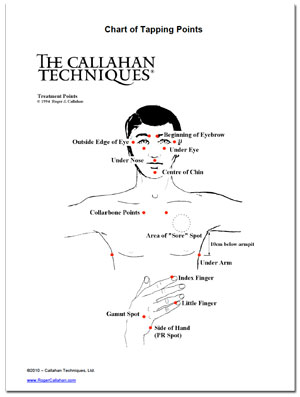
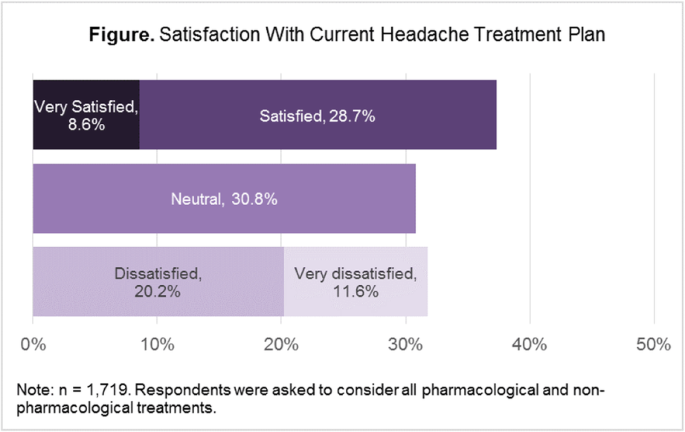
There is universal acceptance in the mental health world, for example, that sexual abuse (in a defined way) is part of the experience of something between 25 and 30% of women before the age of 18. Numerous academic studies support the notion that traumatic events are really quite common. A vulnerability to anxiety may underlie the life interrupting experiences of panic attacks. A vulnerability to addictions may manifest as, for example, problematic drinking. In fact unresolved traumatic stress, amongst other things, can be important in tipping vulnerabilities into symptoms. This is sometimes referred to as sub-syndromal traumatic stress and it is a very useful way thinking about these disturbances. Some things can be very distressing and traumatic for some people that may not affect others in that same way. In preference, let us talk about traumatic stress which includes those who may tick the right boxes for PTSD but it also includes many others who might not tick the right boxes but are still distressed and have the quality of their lives adversely affected. This can be seen as a legal issue more than a mental health issue as to whether one is PTSD or not. In order to be diagnosed with PTSD one needs to exhibit a certain combination of 17 symptoms. Mental health practitioners who find themselves overly oriented towards diagnosis can lose sight of the individuality of the person the idiosyncratic collection of experiences and circumstances that bring the person to the symptoms with which they present.Īn example of this may be the DSM-IV (Diagnostic and Statistical Manual) diagnosis of PTSD (post traumatic stress disorder). This way any relevant and important contributory issues can be considered rather than there being the risk that they can get overlooked or even ignored. A cynical view here could be that this can amount to a pigeon holing of clients and a subsequent railroading of treatment.Ī person centred approach rather than a diagnosis driven treatment plan can mean that a more open view of the whole person in the context of their life history can be considered. Many mental health practitioners appear to approach the provision of care to their clients from a standpoint of applying a diagnosis which then points them in the direction of various treatment approaches relating to the diagnosis. You’re coping quite well until bang – the pancake stack topples and you just can’t function as well as you would like let alone see yourself going anywhere else but further down. Where things seem to be consistently not going well, there may be not just one but many unresolved life issues that have stacked up one on top of the other - on top of the next like a precariously balanced pile of pancakes. Think back again to the memory you just brought to mind and consider whether what you do or how you do what you do could be driven by underlying unresolved life issues. How are you processing what’s going on for you - right now: With a optimistic attitude or with a negative bent? Now consider your frame of mind – right now: Are things going really well for you or, perhaps, not so well. What is the first one that pops into your head? Is it a strong memory? Is it a good memory or is it a bad one? We are who we are and we do the things we do based on the residual effects of the things, circumstances and memories of our past.Ĭlose your eyes for a minute and think of a memory. Our collection of life experiences contributes to the making of us. Sounds like a song title doesn’t it? But seriously have you ever wondered why we do the things we do?
- Blog
- Icloud Generator V3.2.1
- Chupulu Kalasina Subhavela Serial All Episodes
- Doraemon Episodes In Hindi 2012 Free Download
- Bacaan Doa Sholat Tahajud Pdf
- Medison Sa 600 Manual
- Intel Q35 Chipset Host Embedded Controller Interface Driver
- Animezeria One Piece Season 17
- Descargar Libro Cloud Atlas Espanol Pdf
- Vag-Com Release 409.1 For Modern Serial Interfaces
- Dell Sigmatel Audio Driver Windows 7
- Download Download Tunerpro Definition Files Free
- Baixar Driver De Rede Realtek Nicdrv_8169 Win7
- Install Solaris On Kvm Qemu
- Boldbeast Call Recorder Cracked Version Of Snapchat
- American Pie Hindi Dubbed Movie Download
- How To Pass Japanese Drivers Test
- 24 Mani Neram Tamil Movie Mp3 Songs Free Download
- Remove Xml Version= 1.0 Encoding= Utf-8 From Xml C#
- Windows 98 Nes Rom Download
- Castlevania Rondo Of Blood Snes Rom
- Venkatachalapathy Mp3 Songs In Tamil
- Hayley Westenra Paradiso Rar File
- Vamsam Serial Roja Facebook
- Mailbox Has Been Temporarily Moved On Microsoft Exchange Server
- Body By Science Mcguff Pdf Creator
- Rgh xbox one 2016
- Epson wf 3640 driver
- Wansview app on multi pcs
- Arkaos grand vj 1-2
- Xiaopan os
- Thought field therapy migraine algorithm
- Dr cleaner pro cracked
- Uberstrike shotgun
- Refurbished flip video camera
- Voicemod pro free 2021
- Mario kart 8 best kart
- Jinke marina song
